Bursitis Of The Foot Inflammed Joints
Achilles tendon bursitis occurs mainly in young women but can develop in men. Walking in a way that repeatedly presses the soft tissue behind the heel against the stiff back support of a shoe can cause or aggravate the bursitis. Shoes that taper sharply inward toward the posterior heel (such as high-heeled shoes) can cause irritating pressure that leads to the development of this bursitis. Normally, only one bursa is in the heel, between the Achilles tendon and the heel bone (calcaneus). This bursa may become inflamed, swollen, and painful, resulting in anterior Achilles tendon bursitis. Abnormal pressure and foot dysfunction can cause a protective bursa to form between the Achilles tendon and the skin. This bursa may also become inflamed, swollen, and painful, resulting in posterior Achilles tendon bursitis. Any condition that puts extra strain on the Achilles tendon can cause anterior Achilles tendon bursitis. Injuries to the heel and diseases such as rheumatoid arthritis can also cause it.
Causes
Pain at the posterior heel or ankle is most commonly caused by pathology at either the posterior calcaneus (at the calcaneal insertion site of the Achilles tendon) or at its associated bursae. Two bursae are located just superior to the insertion of the Achilles (calcaneal) tendon. Anterior or deep to the tendon is the retrocalcaneal (subtendinous) bursa, which is located between the Achilles tendon and the calcaneus. Posterior or superficial to the Achilles tendon is the subcutaneous calcaneal bursa, also called the Achilles bursa. This bursa is located between the skin and posterior aspect of the distal Achilles tendon. Inflammation of either or both of these bursa can cause pain at the posterior heel and ankle region.
Symptoms
Pain and tenderness are common symptoms. If the affected joint is close to the skin, as with the shoulder, knee, elbow, or Achilles tendon, swelling and redness are seen and the area may feel warm to the touch. The bursae around the hip joint are deeper, and swelling is not obvious. Movement may be limited and is painful. In the shoulder, it may be difficult to raise the arm out from the side of the body. Putting on a jacket or combing the hair becomes a troublesome activity. In acute bursitis symptoms appear suddenly, with chronic bursitis, pain, tenderness, and limited movement reappear after exercise or strain.
Diagnosis
When you suspect you have retrocalcaneal bursitis, your foot doctor will begin by taking a complete history of the condition. A physical exam will also be performed. X-rays are usually taken on the first visit as well to determine the shape of the heel bone, joint alignment in the rearfoot, and to look for calcium deposits in the Achilles tendon. The history, exam and x-rays may sufficient for your foot surgeon to get an idea of the treatment that will be required. In some cases, it may be necessary to get an ultrasound or MRI to further evaluate the Achilles tendon or its associated bursa. While calcium deposits can show up on xray, the inflammation in the tendon and bursa will show up much better on ultrasound and MRI. The results of these tests can usually be explained on the first visit. You can then have a full understanding of how the problem started, what you can do to treat prevent it from getting worse/ You will also know which treatment will be most helpful in making your heel pain go away.
Non Surgical Treatment
If you follow these steps, most attacks of bursitis should subside in four or five days and all symptoms should be gone within two weeks. Rest the body part that hurts. If you suspect that one activity has caused the pain, stop it until the pain is entirely gone. A sling, splint, or padding may be needed to protect the area from possible bumps or irritation. Try over-the-counter pain relievers. Nonprescription NSAIDs (aspirin, ibuprofen, and naproxen) will help reduce pain and swelling, though they won?t accelerate healing. Acetaminophen will help with pain but it doesn?t reduce inflammation. Ice it, then heat it. Apply ice packs during the first two days to bring down swelling. Then use heat-warm baths or a heating pad (on a medium or low setting)-to ease pain and stimulate blood flow. Don?t push it. Resume exercising only after you feel better. Start with gentle activity. Skip the liniments. Liniments and balms are no help for bursitis. Liniments don?t penetrate deeply enough to treat bursitis, they mainly warm the skin and make it tingle, thus distracting attention from the pain beneath. Massage is likely to make matters worse. Undergo physical therapy. Physical therapy strengthens joint muscles that have been affected by bursitis and may help prevent the bursitis from getting worse.
Surgical Treatment
Surgery. Though rare, particularly challenging cases of retrocalcaneal bursitis might warrant a bursectomy, in which the troublesome bursa is removed from the back of the ankle. Surgery can be effective, but operating on this boney area can cause complications, such as trouble with skin healing at the incision site. In addition to removing the bursa, a doctor may use the surgery to treat another condition associated with the retrocalcaneal bursitis. For example, a surgeon may remove a sliver of bone from the back of the heel to alter foot mechanics and reduce future friction. Any bone spurs located where the Achilles attaches to the heel may also be removed. Regardless of the conservative treatment that is provided, it is important to wait until all pain and swelling around the back of the heel is gone before resuming activities. This may take several weeks. Once symptoms are gone, a patient may make a gradual return to his or her activity level before their bursitis symptoms began. Returning to activities that cause friction or stress on the bursa before it is healed will likely cause bursitis symptoms to flare up again.
Foot Pain After Hammertoe Surgery
 Overview
Overview
A hammertoe is a deformity in the foot, causing the second, third, or fourth toe to be permanently bent in the middle joint, causing the toe Hammer toes to resemble a hammer (hence, its name!) or a claw. They are most commonly found in women who wear narrow shoes, such as high heels, that cause the toes to bend unnaturally for extended periods of time. A hammertoe may be difficult or painful to move, and the skin may become callused from rubbing against the inside of the shoe. In fact, there are two types of hammertoe: flexible and rigid. Flexible hammertoes can still move at the joint and are indicative of an earlier, milder form of the problem. Rigid hammertoes occur when the tendon no longer moves, and at this stage, surgery is usually necessary to fix the problem.
Causes
Many people develop hammertoe because they wear shoes that are too tight. Shoes with narrow toe boxes squeeze the toes together, forcing some to bend. This causes the toe muscles to contract. If the toes are forced into this cramped position too often, the muscles may permanently tighten, preventing the toes from extending. Chronic hammertoe can also cause the long bones that connect the toes to the foot, called metatarsals, to move out of position. The misaligned metatarsal bones may pinch a nerve running between them, which can cause a type of nerve irritation called a neuroma.
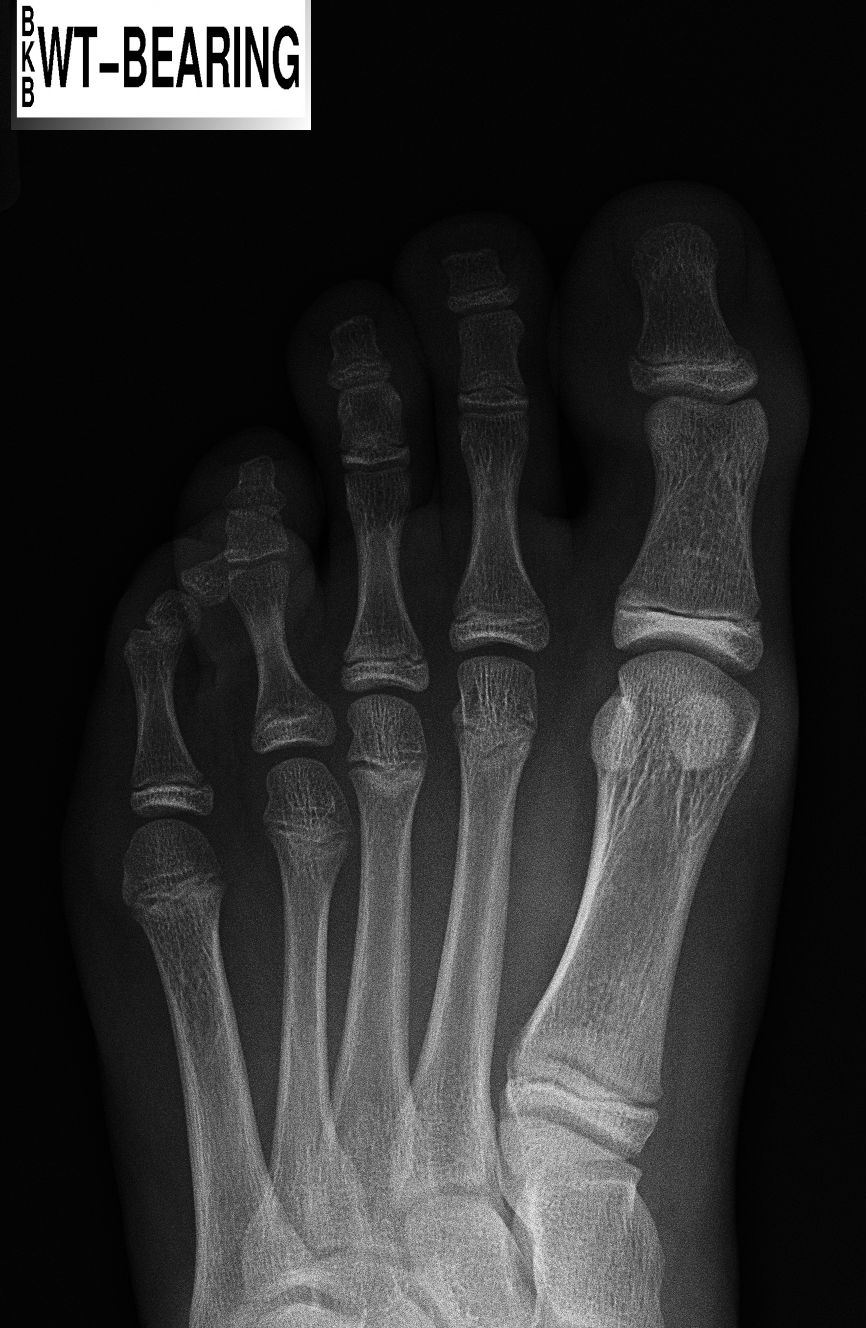 Symptoms
Symptoms
Common symptoms of hammertoes include pain or irritation of the affected toe when wearing shoes. corns and calluses (a buildup of skin) on the toe, between two toes, or on the ball of the foot. Corns are caused by constant friction against the shoe. They may be soft or hard, depending upon their location. Inflammation, redness, or a burning sensation. Contracture of the toe. In more severe cases of hammertoe, open sores may form.
Diagnosis
The treatment options vary with the type and severity of each hammer toe, although identifying the deformity early in its development is important to avoid surgery. Your podiatric physician will examine and X-ray the affected area and recommend a treatment plan specific to your condition.
Non Surgical Treatment
If you have hammer toe, avoiding tight shoes and high heels may provide relief. Initial (non-surgical) treatment for hammer toe involves wearing shoes with plenty of room in the toe area. Shoes should be at least one-half inch longer than the longest toe. Stretching and strengthening exercises for the toes (such as picking up items with the toes or stretching the toes by hand) are also recommended. Sometimes orthopedists recommend special pads, cushions, or slings to help relieve the pain of hammer toe.
Surgical Treatment
In advanced cases in which the toe has become stiff and permanently bent, the toe can be straightened with surgery. One type of surgery involves removing a small section of the toe bone to allow the toe to lie flat. Surgery for hammertoe usually is classified as a cosmetic procedure. Cosmetic foot surgeries sometimes result in complications such as pain or numbness, so it's better to treat the problem with a shoe that fits properly.
 Prevention
Prevention
The key to prevention is to wear shoes that fit you properly and provide plenty of room for your toes. Here?s how to get the right fit. Have your feet properly measured. The best way to do this is to get someone to draw the outline of your foot while you stand barefoot with your full weight on it, then measure the outline at the widest point. Measure the soles of your shoes. Ideally, they should be as wide as your feet, but certainly no more than half an inch narrower. Length matters, too, of course: your shoes should be half an inch longer than your longest toe.
Hammertoe Pain Relief
 Overview
Overview
There are two main types of hammertoe. Hammertoes can be flexible, which means that you can still move the toe a bit - these are easier to treat with stretching, wider shoes and in some cases, toe splints. Rigid hammertoes occur when the foot condition has persisted for so long without treatment that the tendons become too rigid to be stretched back to normal. Rigid hammertoes are more common in people with arthritis. This foot condition usually needs to be treated with surgery.
Causes
The main cause of hammer toe is poorly fitted and/or poorly designed footwear. Any footwear that is too tight in the hammertoe toe box, especially high-heeled shoes, can push the toes forward, crowding one or more of them into a space that is not large enough to allow the toes to lie flat and spread as they should. Other causes include the following. Changes in foot anatomy. Sometimes the metatarsal bones in the ball of the foot can ?drop,? creating a situation in which the toes do not make contact with the surface of the shoe. The toes may then contract at one or both of the joints to re-establish contact with the surface. Traumatic injuries in which toes are jammed or broken. Diabetic neuropathy. This can cause abnormal foot biomechanics due to nerve and/or muscle damage. Damage to nerves and muscles from other conditions, such as arthritis or stroke. Heredity.
 Symptoms
Symptoms
The symptoms of a hammer toe include the following. Pain at the top of the bent toe upon pressure from footwear. Formation of corns on the top of the joint. Redness and swelling at the joint contracture. Restricted or painful motion of the toe joint. Pain in the ball of the foot at the base of the affected toe.
Diagnosis
The exam may reveal a toe in which the near bone of the toe (proximal phalanx) is angled upward and the middle bone of the toe points in the opposite direction (plantar flexed). Toes may appear crooked or rotated. The involved joint may be painful when moved, or stiff. There may be areas of thickened skin (corns or calluses) on top of or between the toes, a callus may also be observed at the tip of the affected toe beneath the toenail. An attempt to passively correct the deformity will help elucidate the best treatment option as the examiner determines whether the toe is still flexible or not. It is advisable to assess palpable pulses, since their presence is associated with a good prognosis for healing after surgery. X-rays will demonstrate the contractures of the involved joints, as well as possible arthritic changes and bone enlargements (exostoses, spurs). X-rays of the involved foot are usually performed in a weight-bearing position.
Non Surgical Treatment
You can usually use over-the-counter cushions, pads, or medications to treat bunions and corns. However, if they are painful or if they have caused your toes to become deformed, your doctor may opt to surgically remove them. If you have blisters on your toes, do not pop them. Popping blisters can cause pain and infection. Use over-the-counter creams and cushions to relieve pain and keep blisters from rubbing against the inside of your shoes. Gently stretching your toes can also help relieve pain and reposition the affected toe.
Surgical Treatment
In advanced cases in which the toe has become stiff and permanently bent, the toe can be straightened with surgery. One type of surgery involves removing a small section of the toe bone to allow the toe to lie flat. Surgery for hammertoe usually is classified as a cosmetic procedure. Cosmetic foot surgeries sometimes result in complications such as pain or numbness, so it's better to treat the problem with a shoe that fits properly.
How To Cure Bunions
Overview
If you have bunions, taking care of them now can help you avoid more serious treatment later. A bunion is a bump that forms on the joint of the big toe when bone or tissue moves out of place and extends beyond the normal anatomy of the toe. Left untreated, bunions can cause debilitating pain and may require surgery to correct.
Causes
Bunions most commonly affect women. Some studies report that bunions occur nearly 10 times more frequently in women. It has been suggested that tight-fitting shoes, especially high-heel and narrow-toed shoes, might increase the risk for bunion formation. Bunions are reported to be more prevalent in people who wear shoes than in barefoot people. While the precise causes are not known, there also seems to be inherited (genetic) factors that predispose to the development of bunions, especially when they occur in younger individuals. Other risk factors for the development of bunions include abnormal formation of the bones of the foot at birth (congenital), nerve conditions that affect the foot, rheumatoid arthritis, and injury to the foot. Bunions are common in ballet dancers.
Symptoms
Most patients complain of pain directly on the bunion area, within the big toe joint, and/or on the bottom of the foot. The bunion may become irritated, red, warm, swollen and/or callused. The pain may be dull and mild or severe and sharp. The size of the bunion doesn?t necessarily result in more pain. Pain is often made worse by shoes, especially shoes that crowd the toes. While some bunions may result in significant pain, other bunions may not be painful at all.
Diagnosis
Your doctor will be able to diagnose a bunion by asking about your symptoms and examining your feet. You may also have blood tests to rule out any other medical conditions, such as rheumatoid arthritis or gout, although this is rare. Your doctor may refer you to a podiatrist or chiropodist (healthcare professionals who specialise in conditions that affect the feet).
Non Surgical Treatment
Several things can be done to help relive the pain of bunions. These won't make the bunion go away, but they can make the foot more comfortable. Wearing different shoes. Shoes with a wide toe box rather than a pointed one will help. Shoes with lower heels will also help. (High heels throw more of the body's weight on the front part of the foot where the toe joints are.) Padding. Pads placed over the bunion may help reduce the pain. These are available from a drug store or may be available from a foot and ankle surgeon. Avoiding activities that make the pain worse. This includes standing for a long time or other activities that make the bunion sore. Non-steroidal anti-inflammatory drugs. These include aspirin or ibuprofen. They relieve pain and swelling. Applying an ice pack to reduce swelling and pain. Corticosteroid injections. These are not often used in bunion treatment. Injecting corticosteroids sometimes helps if the bursa is inflamed. (Bursa is a fluid-filled sac within a joint to cushion the bones). Orthotic devices. These are devices placed inside a shoe that shift the positioning of the foot. Orthotics help compensate for structural issues that cause foot problems. 
Surgical Treatment
When a surgeon cuts and repositions a bone, it is referred to as an osteotomy. There are two basic techniques used to perform an osteotomy to realign the first metatarsal. In some cases, the far end of the bone is cut and moved laterally (called a distal osteotomy). This effectively reduces the angle between the first and second metatarsal bones. This type of procedure usually requires one or two small incisions in the foot. Once the surgeon is satisfied with the position of the bones, the osteotomy is held in the desired position with one, or several, metal pins. Once the bone heals, the pin is removed. The metal pins are usually removed between three and six weeks following surgery. In other situations, the first metatarsal is cut at the near end of the bone (called a proximal osteotomy). This type of procedure usually requires two or three small incisions in the foot. Once the skin is opened the surgeon performs the osteotomy. The bone is then realigned and held in place with metal pins until it heals. Again, this reduces the angle between the first and second metatarsal bones. Realignment of the big toe is then done by releasing the tight structures on the lateral, or outer, side of the first MTP joint. This includes the tight joint capsule and the tendon of the adductor hallucis muscle. This muscle tends to pull the big toe inward. By releasing the tendon, the toe is no longer pulled out of alignment. The toe is realigned and the joint capsule on the side of the big toe closest to the other toe is tightened to keep the toe straight, or balanced. Once the surgeon is satisfied that the toe is straight and well balanced, the skin incisions are closed with small stitches. A bulky bandage is applied to the foot before you are returned to the recovery room.
Prevention
There are some steps that may help prevent, or at least slow, the progression of bunions. Avoid shoes with a narrow toe box. If your foot flattens excessively, make sure you wear supportive shoes, and if necessary, get custom orthotics from your podiatrist. See your podiatrist at the first signs or symptoms of a bunion deformity, as early treatment may stop or slow its progression.
What Causes Over-Pronation Of The Feet
Pronation refers to the inward roll of the foot during normal motion and occurs as the outer edge of the heel strikes the ground and the foot rolls inward and flattens out. A moderate amount of pronation is required for the foot to function properly, however damage and injury can occur during excessive pronation. When excessive pronation does occur the foot arch flattens out and stretches the muscles, tendons and ligaments underneath the foot.

Causes
Over-pronation may happen because the tissue that attaches to your foot bones is loose. You may be born with this problem or it may result from injuries or overuse, like from too much running.
Symptoms
Overpronation can lead to injuries and pain in the foot, ankle, knee, or hip. Overpronation puts extra stress on all the bones in the feet. The repeated stress on the knees, shins, thighs, and pelvis puts additional stress on the muscles, tendons, and ligaments of the lower leg. This can put the knee, hip, and back out of alignment, and it can become very painful.
Diagnosis
Look at the wear on your shoes and especially running trainers; if you overpronate it's likely the inside of your shoe will be worn down (or seem crushed if they're soft shoes) from the extra strain.

Non Surgical Treatment
Although there is no actual cure for over-pronation it is possible to correct or at least reduce this problem. In order to restore our normal foot function an 'orthotic' or orthotic insole device is placed inside the shoes. Orthotics are designed to realign the foot and ankle bones to their natural position. This in turn restores our normal foot function and it helps alleviate not only foot problems but also ailments in other parts of the body i.e. the legs, knees and lower back. In addition to wearing an orthotic, it is recommended to wear supportive shoes, like good quality athletic footwear with a firm heel counter and sufficient flexibility in the forefoot area.
Prevention
With every step we take, we place at least half of our body weight on each foot (as we walk faster, or run, we can exert more than twice our body weight on each foot). As this amount of weight is applied to each foot there is a significant shock passed on to our body. Custom-made orthotics will absorb some of this shock, helping to protect our feet, ankles, knees, hips, and lower back.
Tips On How To Diagnose Severs Disease?
Sever's disease, also called calcaneal apophysitis, is a painful bone disorder that results from inflammation (swelling) of the growth plate in the heel. A growth plate, also called an epiphyseal plate, is an area at the end of a developing bone where cartilage cells change over time into bone cells. As this occurs, the growth plates expand and unite, which is how bones grow.
Causes
Risk Factors For Sever?s Disease. While anyone can get Sever?s Disease, it most commonly affects boys, but may also affect girls. Children ages eight to thirteen. Children involved in high-impact sports like baseball, football and soccer. Kids with forefoot to midfoot misalignment walking patterns. Poor-fitting shoes. Standing for long periods of time. Obesity. Flat feet. A gait that roll inwards.
Symptoms
Sever condition causes pain at the back of the heel. The pain is increased with plantar flexion of the ankle (pushing down with the foot as if stepping on the gas), particularly against resistance. Sever condition also causes tenderness and swelling in the area of the pain.
Diagnosis
A doctor can usually tell that a child has Sever's disease based on the symptoms reported. To confirm the diagnosis, the doctor will probably examine the heels and ask about the child's activity level and participation in sports. The doctor might also use the squeeze test, squeezing the back part of the heel from both sides at the same time to see if doing so causes pain. The doctor might also ask the child to stand on tiptoes to see if that position causes pain. Although imaging tests such as X-rays generally are not that helpful in diagnosing Sever's disease, some doctors order them to rule out other problems, such as fractures. Sever's disease cannot be seen on an X-ray.
Non Surgical Treatment
Depending on the diagnosis and the severity of the pain, there a number of treatment options available. Rest, reduce activity, your child should reduce or stop any activity that causes pain, such as sports and running. This can be a difficult option, as children are normally quite willful in pursuit of their favorite pastimes. Over the counter anti-inflammatory drugs, such as ibuprofen (found in Nurofen), to help reduce pain and inflammation. Make certain your child does stretching exercises before play. This will often help reduce the stress on the fascia and relieve heel pain in your child. Orthotic insoles. Orthotics made for children will help support the foot properly, and help prevent over-pronation or improper gait by supporting your child?s foot into a proper biomechanical position. Do not hesitate to schedule an appointment with a podiatrist, should your child?s heel and foot pain persist.
Achilles Rupture Facts Not Misconceptions
Overview
 The Achilles tendon is found in the back of the leg above the heel, and is the largest tendon in the body. It connects the calf muscles to the heel bone and is used when walking, running and jumping. A rupture of the tendon is a tearing and separation of the tendon fibers. When a rupture of the tendon occurs, the tendon can no longer perform its normal function. A common issue related to a tear is the inability to point your toe.
The Achilles tendon is found in the back of the leg above the heel, and is the largest tendon in the body. It connects the calf muscles to the heel bone and is used when walking, running and jumping. A rupture of the tendon is a tearing and separation of the tendon fibers. When a rupture of the tendon occurs, the tendon can no longer perform its normal function. A common issue related to a tear is the inability to point your toe.
Causes
The Achilles tendon is a strong bands of fibrous connective tissue that attaches the calf muscle to the heel bone. When the muscle contracts, the tendon transmits the power of this contraction to the heel bone, producing movement. The Achilles tendon ruptures because the load applied to it is greater than the tendon's ability to withstand that load. This usually occurs as a result of a sudden, quick movement where there is a forceful stretch of the tendon or a contraction of the muscles eg: jumping, sprinting, or pushing off to serve in tennis. This occurs most often in sports that require a lot of stopping and starting (acceleration-deceleration sports) such as tennis, basketball, netball and squash. The Achilles tendon is on average 15cm in length. Most ruptures occur 2-6cm above where the tendon inserts into the heel bone. This is the narrowest portion of the Achilles tendon and is also the area with the poorest blood supply. achilles tendon rupture is most common when the muscles and tendon have not been adequately stretched and warmed up prior to exercise, or when the muscles are fatigued. the Achilles tendon has a poor blood supply, which makes it susceptible to injury and slow to heal after injury. During exercise the amount of blood able to travel to the tendon is decreased, further increasing the risk of rupture. Most experts agree that there are no warning signs of an impending rupture. However, frequent episodes of Achilles tendonitis (tendon inflammation) can weaken the tendon and make it more susceptible to rupture.
Symptoms
The pain from an Achilles tendon rupture is usually felt in the back of the lower leg, in the area 2 to 6 cm. above the Achilles tendon's attachment to the calcaneus. Individuals with an Achilles tendon rupture often describe a "pop" or similar feeling at the time of the injury. A "hole" or defect in the Achilles tendon can usually be felt under the skin in this area. A limp and inability to rise up on the toes of the affected foot are usually present. If the affected foot does not plantar flex when the calf muscles are squeezed an Achilles tendon rupture is very likely.
Diagnosis
The diagnosis of an Achilles tendon rupture is made entirely on physical examination. Often, there is a substantial defect in the Achilles from 2-5 cm before it inserts into the heel bone. However, the main test is to determine whether the Achilles has been ruptured is the Thompson test. This essentially involves placing the patient on their stomach and squeezing the calf muscle. If the Achilles is intact, the foot will rise [plantar flex]. If it is ruptured, the foot will not move and will tend to be in a lower lying position.
Non Surgical Treatment
Two treatment options are casting or surgery. If an Achilles tendon rupture is untreated then it may not heal properly and could lead to loss of strength. Decisions about treatment options should be made on an individual basis. Non-surgical management traditionally is selected for minor ruptures, less active patients, and those with medical conditions that prevent them from undergoing surgery. The goal of casting is to allow the tendon to slowly heal over time. The foot and ankle are positioned to bring the torn ends of the tendon close together. Casting or bracing for up to 12 weeks or more may be necessary. This method can be effective and avoids some risks, such as infection, associated with surgery. However, the likelihood of re-rupture may be higher with a non-surgical approach and recovery can take longer. 
Surgical Treatment
Surgery could allow for a quicker healing time. The procedure generally involves making an incision in the back of your lower leg and stitching the torn tendon together. Depending on the condition of the tissue, the repair may be reinforced with other tendons. As with any surgery, the main complication is the risk for infection, however, this risk is reduced by using smaller incisions.
Prevention
The following can significantly reduce the risk of Achilles tendon rupture. Adequate stretching and warming up prior to exercising. If playing a seasonal sport, undertake preparatory exercises to build strength and endurance before the sporting season commences. Maintain a healthy body weight. This will reduce the load on the tendon and muscles. Use footwear appropriate for the sport or exercise being undertaken. Exercise within fitness limits and follow a sensible exercise programme. Increase exercise gradually and avoid unfamiliar strenuous exercise. Gradual ?warm down? after exercising.